-
Do You Need Antibiotics?
When you develop an illness, such as a viral infection (i.e. a common cold) or have a superficial wound (like a cut or scratch), these are things that will usually resolve on their own over a few days or couple of weeks, depending on the severity of your illness and the symptoms that you experience. If you have a viral infection, antibiotics will not help resolve your illness or speed up the recovery time. Taking an antibiotic when it is unnecessary to do so will potentially cause antibiotic resistance. However, during your recovery period, there are certain over-the-counter products that can purchase in order to help relieve symptoms. For example,…
-
Overcoming Mental Fatigue
When it comes to overexerting yourself, both the body and mind can be affected. According to psychologists, we all have limits when it comes to our cognition, and when we take on more than what we can handle that can ultimately result in mental fatigue – also known as exhaustion. In fact, it’s one of the reasons why we’re seeing more and more athletes and celebrities being hospitalized, because their scheduled are either too jam packed or they’ve taken on more than their bodies allow. To avoid mental fatigue, it’s important that you not overcommit yourself to things. If you’re being pulled in a million different directions, you’re going to…
-
Tailoring Products to Your Skin Type
When it comes to finding the right skincare products, it’s important to know that everyone’s skin is different and not all products are made to be used universally. For example, you might have more sensitive skin and therefore need to use products that have less ingredients and are free from fragrance, while someone else’s main concern with their skin might not be sensitivity, but instead be fine lines and wrinkles. The type of product you should be using depends on your skin type, which there are 4 of: • Normal skin • Dry skin • Oily skin • Combination skin If you have normal skin, this means that your skin…
-
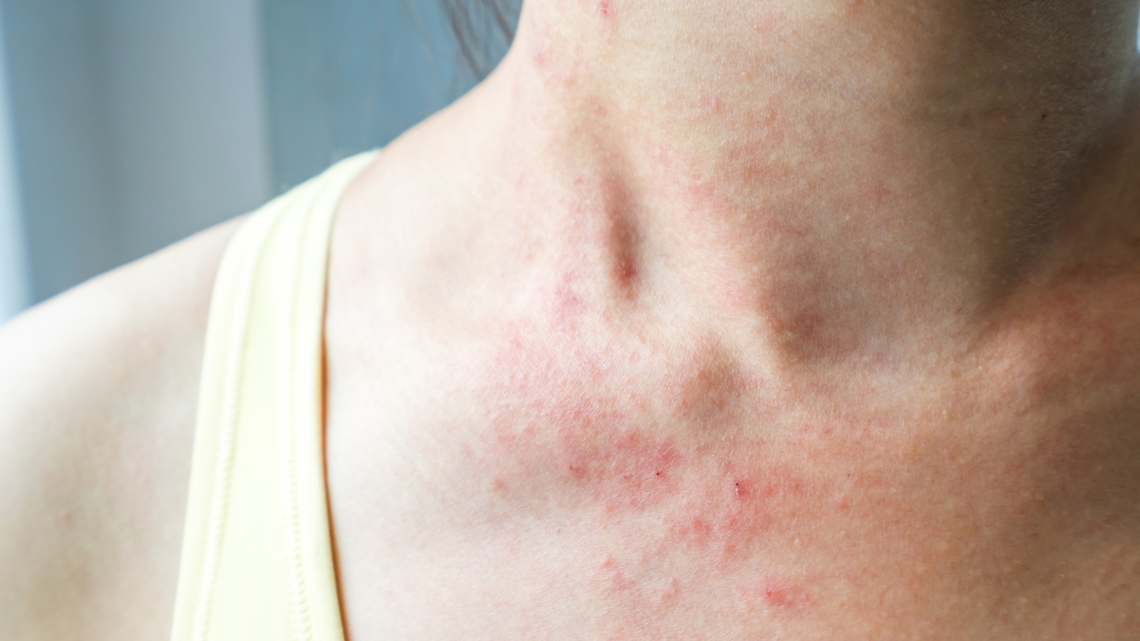
Heat Rash
As the mercury rises and the sun beats down relentlessly during the sweltering summer months, many individuals find themselves grappling with a variety of heat-related health issues. Among these, heat rash stands out as a particularly common and bothersome condition that affects people of all ages, from infants to the elderly. Also known as miliaria or prickly heat, this dermatological ailment can turn an otherwise enjoyable summer day into an uncomfortable and irritating experience. In this extensive article, we will delve deep into the world of heat rash, exploring its causes, symptoms, treatment options, and preventive measures, all while shedding light on why this condition becomes so prevalent during the…
-
Recognizing the Signs of Dehydration
Dehydration is a condition that occurs when the body loses more fluids than it takes in, resulting in an inadequate amount of water and other fluids necessary for normal bodily functions. Water is essential for a variety of physiological processes, including maintaining cellular structure, regulating body temperature, and enabling the transportation of nutrients and waste products. Given that the human body is composed of approximately 60% water, the significance of maintaining adequate hydration levels cannot be overstated. In this comprehensive article, we will explore the various signs of dehydration, the physiological mechanisms underlying this condition, and its potential impact on health. By understanding the signs of dehydration and the importance…
-
Health Lessons Learned from 2021 Heat Dome
The heat dome that struck British Columbia in June and July of 2021 was a catastrophic event that claimed the lives of 619 people, a stark reminder of the increasing frequency and severity of extreme weather events due to climate change. This phenomenon, which is characterised by a high-pressure system that traps warm air underneath it, led to unprecedented temperatures, with some areas recording highs of nearly 50 degrees Celsius. The consequences were devastating, not only in terms of human lives lost but also in the strain placed on healthcare services, infrastructure, and the environment. Heat-related illnesses can range from mild conditions like heat exhaustion to severe, life-threatening conditions such…
-
Summer’s Heat: Health Risks and Impacts
The human body is remarkably adept at regulating its internal temperature, but extreme heat can overwhelm these mechanisms, leading to a range of health issues. When ambient temperatures rise, our bodies respond by increasing blood flow to the skin and producing sweat to facilitate evaporative cooling. However, these processes can be compromised in certain conditions, such as high humidity or dehydration, potentially resulting in heat-related illnesses. One of the most common heat-related health concerns is heat exhaustion. This condition occurs when the body loses excessive amounts of water and salt through sweating. Symptoms of heat exhaustion include heavy sweating, weakness, dizziness, headache, nausea, and muscle cramps. If left untreated, heat…
-
Common Summer Health Hazards
Warmer weather can be a nice break from all the rain we’re used to getting in Vancouver, but there are also certain hazards that come along with the summer and heat. Find out what some of those are below, along with what precautions you should take to protect yourself. Dehydration Staying hydrated is important. Not just during the summer months, but all the time. Drinking water not only keeps you hydrated and helps regulate body temperature, but it also increases energy levels and helps with muscle performance. Unfortunately, summer is a season where it’s not uncommon for physicians to see patients presenting with symptoms of dehydration – usually due to…
-
Healthy Foods to Eat in the Summer
When it’s warm out, the last thing anyone wants to do is stand over a hot oven or stove cooking – and the warmer the weather, the more tempting it can be to want to grab something quick and easy, which might not always be the healthiest. For example, getting something from a fast food restaurant, which could be loaded with grease, bad carbohydrates and sugar – all things you want to avoid to ensure optimal health and reduce the risk of potential health problems like weight gain, diabetes, and cardiovascular disease. Before we dive into the topic of food, it’s a good time to remind everyone about the importance…
-
Sleeping Comfortably in the Summer
For those who suffer from insomnia, you know how hard falling asleep (and staying asleep!) can be. For those of you who don’t suffer from insomnia, getting a good night’s rest can still be difficult – especially on nights as hot as the ones we’ve been experiencing in Vancouver lately. So what do you do if you’re finding it too uncomfortable to get that desperately needed shut-eye? Check out some helpful tips and tricks below. Air Conditioning If you’re looking for a quick cool-down, crank up the A/C. Of course this is the obvious answer, but unfortunately not everyone has (or can afford) an air conditioning unit; while others who…