-
Home Health and Safety
Your home can be a place of comfort, but it can also be a place of things such as stress, indoor air pollution, germs, and other health hazards. In this article, you’ll find information on how to give your house the healthiest makeover possible, and how making just a few simple changes can benefit you and your family’s overall health and wellness in the long-run. The Kitchen There are many different hazards in the kitchen that we don’t often think about. Everything from how to handle and cook our food, to cleaning the dishes. When it comes to cooking things such as meat and poultry, we need to be extra…
-
Joint Health: Common Disorders and Prevention
The joints are what form the connections between your bones and provide your body with support as well as help you move. When your joints become damaged, that movement is interfered and can result in pain. As for what causes damage to the joints, there are a number of reasons – though the most common include disease or injury. Below we take a look at a few of the specific joint-related diseases and injuries in depth, and what you can do to prevent them or find relief. Osteoarthritis OA is one of the most common disorders of the joints that people are diagnosed with. It occurs when the cartilage between…
-
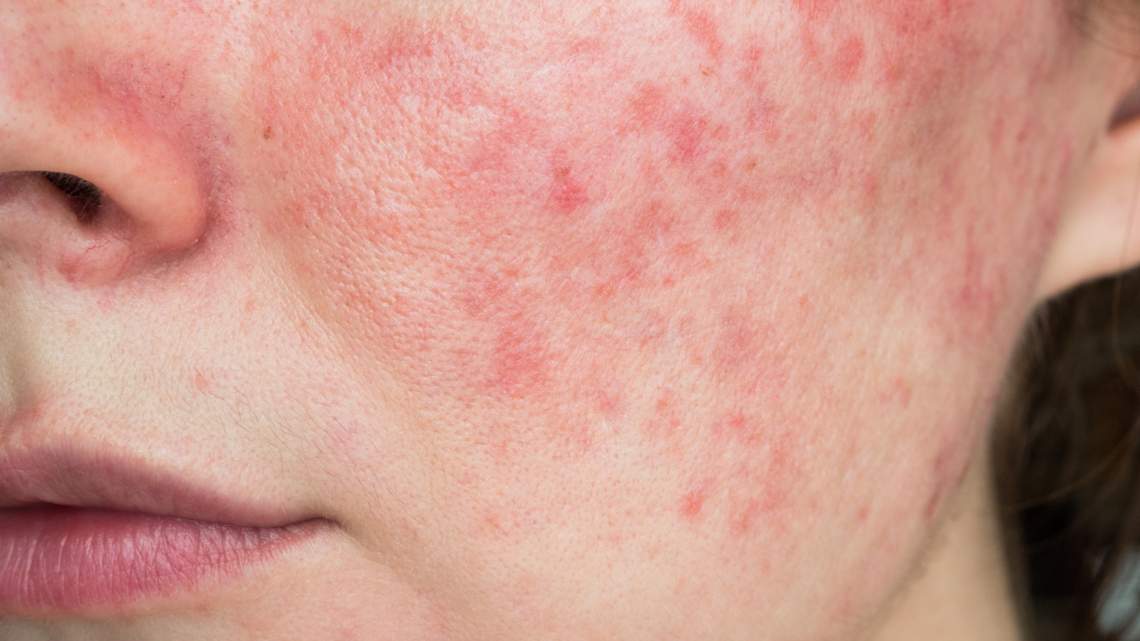
Stress and its Impact on Our Skin
If you’ve noticed recent acne breakouts or other abnormalities with the skin on your face (such as increased redness, psoriasis or eczema) that you don’t normally experience, there is a strong possibility that those breakouts could actually be caused by stress. This is because when you are stressed, two specific hormones known as cortisol and adrenaline increase, causing inflammation as well as contributing to the aggravation of many of the aforementioned skin conditions – in addition to decreased elasticity of the skin and an increase in lines and wrinkles. In general, stress can wreak havoc on the body, but there are certain things you can do to find relief and…
-
Anxiety Disorders in Canada
In 2022, data revealed that over 5 million Canadians aged 18 or older met the diagnostic criteria for a mood, anxiety, or substance use disorder, a staggering number that highlights the pressing mental health challenges facing the nation. This statistic underscores the pervasive nature of mental health disorders in Canada and the urgent need for comprehensive understanding, effective treatment, and robust support systems to address these issues. The prevalence of these disorders can be attributed to a complex interplay of genetic, environmental, and societal factors, each contributing to the overall mental health landscape in Canada. It is essential to delve deeper into the most common forms of anxiety disorders, their…
-
The Science-Backed Benefits of Protein
Protein is considered one of the most important food elements (also known as a macronutrient) for the normal, healthy growth of the human body, and there are many science-backed reasons as to why you should eat more of it. Your hair and your nails, for example, are made up of mostly protein. Your body also needs protein to create hormones, enzymes and other types of chemicals, and is essential in the building of our muscles, bones, cartilage, blood and skin. While most people consume enough protein to avoid becoming deficient in it, it’s never a bad idea to increase your protein intake – as whether you’re wanting to lose weight…
-
Choosing the Right Footwear
With summer just a couple of weeks away, Vancouver residents are starting to spend more and more time outdoors – especially when it pertains to their physical activity. Regardless of what it is you’re doing to stay fit (whether it’s running, jogging, walking, or partaking in outdoor sports), it’s important to ensure that you have good footwear…because what’s on your feet plays a much bigger role in your health than you might realize. Aside from the obvious (sore feet and blisters), lack of good footwear can also lead to problems with posture and your back. When it comes to choosing the right shoes (especially running shoes), there are some common…
-
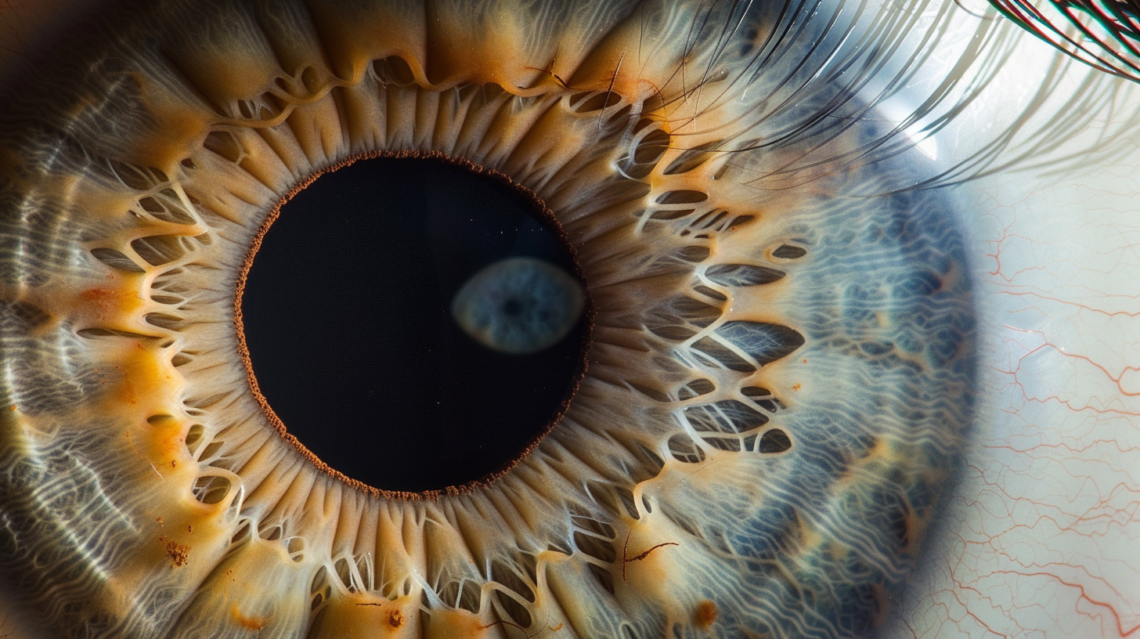
Eye Exams Key to Early Cataract Detection
Cataracts, a condition characterized by the clouding of the lens in the eye, affects more than 2.5 million Canadians. This number is projected to rise to an estimated 5 million by the year 2031. Cataracts are currently the second leading cause of blindness in Canada, surpassed only by age-related macular degeneration. Cataract development is generally a slow and progressive process, often leading to a gradual and painless decrease in vision. This slow progression can make it difficult for individuals to notice changes in their vision immediately, which underscores the necessity of regular eye check-ups to detect and treat cataracts at an early stage. One of the most common initial symptoms…
-
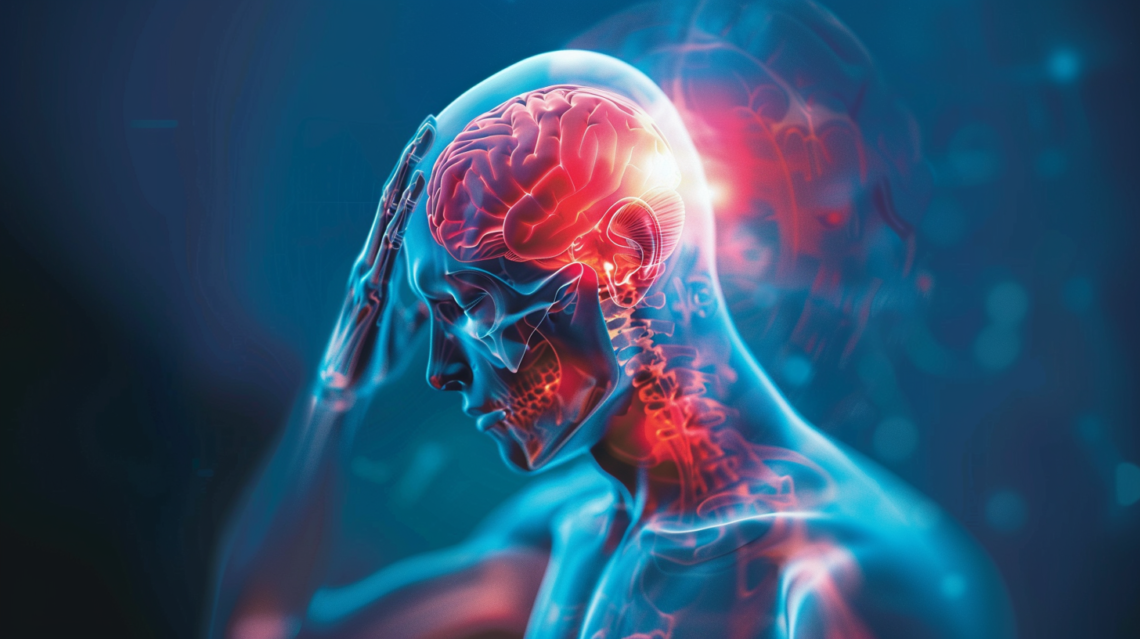
Brain Injuries in Canada
Traumatic brain injury (TBI) represents one of the most significant public health concerns in Canada. By 2031, TBI is expected to be among the most prevalent neurological conditions affecting Canadians, alongside Alzheimer’s disease, other dementias, and epilepsy. The impact of TBI on individuals and society is profound, given its role as a leading cause of disability both globally and domestically. In Canada, approximately 2% of the population lives with a TBI, leading to about 18,000 hospitalizations annually. One-third of these individuals are women, with a notable prevalence of TBI during the early reproductive years (15-24 years), primarily due to intimate partner violence and accidents. Women with TBI are also more…
-
Nutritional Strategies for Stress Reduction
Stress can impact us in a number of ways and for a number of different reasons. There are also many different ways to deal with stress, including everything from trying different relaxation techniques to speaking with a counsellor. Stress can also be a common contributor to both anxiety and panic attacks, which sometimes need to be managed with medication. What you might not be aware of, however, is the role your diet can also play when it comes to stress management. When you’re stressed out, your body produces hormones that can cause a temporary increase in your blood pressure. If your high blood pressure is, in fact, related to stress,…
-
The Connection Between Body and Mind
Exercise has long been recognized as an essential component of physical health. From improving cardiovascular endurance to increasing muscle strength, the benefits of regular physical activity are well-established. However, the impact of exercise on mental wellbeing is a topic that deserves equal attention. This article delves into the multifaceted relationship between exercise and mental wellbeing, shedding light on how physical activity can enhance emotional resilience and cognitive function while preventing mental health disorders. The Science Behind Exercise and Mental Wellbeing To better understand the connection between exercise and mental wellbeing, it’s crucial to recognize the physiological processes that underlie this relationship. When we engage in physical activity, our body responds…